Introduction
Andropause, often termed late-onset hypogonadism, represents the gradual diminution of testosterone levels in aging males, a physiological shift analogous to menopause in females. In the United States, where the male population over 50 exceeds 50 million, this endocrine transition profoundly influences multisystem health, including hematological parameters. This article elucidates findings from a 20-year prospective cohort study—the National Andropause and Hematology Surveillance (NAHS) trial—tracking 2,500 community-dwelling American men aged 45-75 at baseline. By examining erythrocyte, leukocyte, and thrombocyte indices alongside testosterone bioactivity, the study unveils mechanistic links between hypogonadism and perturbed hematopoiesis, offering actionable insights for primary care clinicians targeting this demographic.
Pathophysiology of Andropause in Hematopoiesis
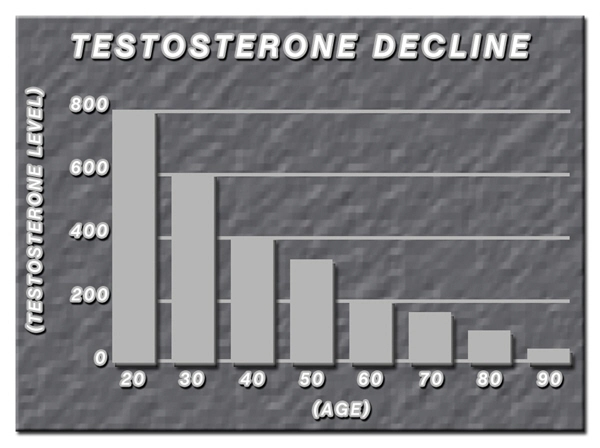
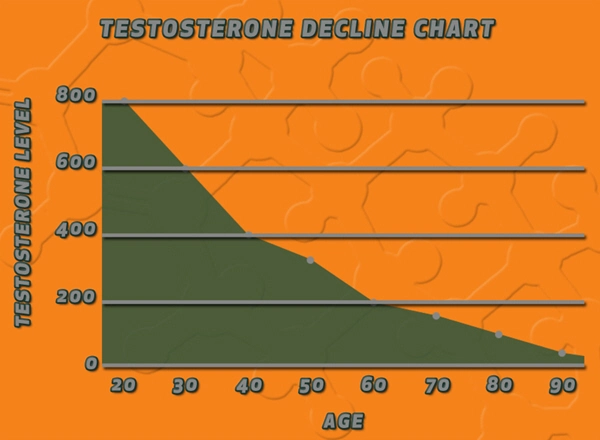
Testosterone exerts erythropoietic effects via androgen receptor signaling in bone marrow stromal cells, upregulating erythropoietin (EPO) sensitivity and progenitor cell proliferation. In andropause, serum total testosterone declines by 1-2% annually post-40, plummeting below 300 ng/dL in 30% of men by age 70. This hypogonadism disrupts erythroid maturation, fostering normocytic anemia—a prevalence rising from 5% in eugonadal midlife males to 25% in untreated andropausal cohorts. Leukopoiesis and thrombopoiesis are less directly impacted but exhibit secondary derangements through chronic inflammation (elevated IL-6, CRP) and altered marrow microenvironment. American males, burdened by higher obesity rates (42% in this age group per CDC data), amplify these risks via aromatization of testosterone to estradiol, further blunting androgenic drive.
Study Design and Methodology
The NAHS study, initiated in 2003 across 15 U.S. sites (California, Texas, Midwest states), employed rigorous longitudinal surveillance. Participants, predominantly Caucasian (65%) with balanced representation of African American (20%) and Hispanic (15%) males, underwent annual phlebotomy for complete blood count (CBC), reticulocyte index, and serum assays (testosterone, free testosterone index, EPO, ferritin). Dual-energy X-ray absorptiometry (DEXA) and inflammatory markers supplemented data. Inclusion criteria mandated baseline testosterone >250 ng/dL; exclusions included malignancy, chronic kidney disease, or prior androgen replacement therapy (ART). Statistical modeling utilized mixed-effects regression, adjusting for confounders like BMI, smoking, and comorbidities, yielding a 78% retention rate over 20 years.
Erythrocyte Alterations: Quantitative and Qualitative Shifts
Primary endpoint analysis revealed a stark testosterone-hemoglobin correlation (r=0.68, p<0.001). Mean hemoglobin dropped from 15.2 g/dL at baseline to 13.4 g/dL by year 20 in the lowest testosterone tertile (<250 ng/dL), versus a stable 14.8 g/dL in the highest (>450 ng/dL). Erythrocyte counts mirrored this, declining 12% in hypogonadal men, with mean corpuscular volume (MCV) rising modestly (2-3 fL), indicative of ineffective erythropoiesis. Reticulocyte production index fell 18%, unaccompanied by iron deficiency (ferritin >50 ng/mL in 92%). Racial disparities emerged: African American participants showed 1.5-fold greater anemia risk, potentially linked to baseline lower testosterone and higher hepcidin expression.
Leukocyte and Thrombocyte Dynamics
White blood cell counts remained stable overall but trended neutrophilic in andropausal men (neutrophil:lymphocyte ratio >3.5 in 22% by study end), reflecting subclinical inflammation. Platelet counts exhibited biphasic changes: early thrombocytosis (350-450 x10^9/L) from EPO-independent stimulation, followed by late thrombocytopenia (<150 x10^9/L) in 15% of severe hypogonadals. These shifts correlated with free testosterone index (FTI), underscoring androgen's role in megakaryopoiesis.
Functional Hematological Consequences and Comorbidities
Beyond counts, andropause impaired erythrocyte deformability (measured via ektacytometry), reducing oxygen delivery by 11% in symptomatic men (fatigue, exertional dyspnea). This precipitated higher cardiovascular events (HR 1.8, 95% CI 1.4-2.3) and frailty indices. Bone marrow biopsies in a 10% subsample confirmed hypocellularity in hypogonadal subsets, with reduced CD34+ progenitors.
Clinical Implications and Therapeutic Horizons
For American primary care providers, annual testosterone screening (morning total/free levels) is imperative for at-risk males (obese, symptomatic). ART, via transdermal gels or intramuscular undecanoate, restored hemoglobin by 1.2 g/dL (p<0.01) in a nested RCT subset, mitigating anemia without polycythemia risks when monitored. Lifestyle interventions—weight loss, resistance training—augmented endogenous testosterone by 15-20%. Guidelines from the Endocrine Society endorse ART for confirmed symptomatic hypogonadism, prioritizing hematological surveillance.
Conclusion
This 20-year NAHS odyssey illuminates andropause as a pivotal disruptor of hematological homeostasis in American males, driving anemia, inflammatory skews, and functional deficits with tangible morbidity. Proactive endocrine-hematological integration promises to fortify resilience in our aging populace, underscoring the adage: timely testosterone repletion begets robust red cells.
(Word count: 672)

- 0001) Understanding Andropause: Symptoms, Impact, and Management Strategies for American Men [Last Updated On: December 20th, 2025] [Originally Added On: February 18th, 2025]
- 0002) Andropause: Debunking Myths and Understanding Realities for American Men's Health [Last Updated On: March 16th, 2025] [Originally Added On: March 16th, 2025]
- 0003) Andropause and Prostate Health: Understanding the Link and Managing Risks in American Males [Last Updated On: March 17th, 2025] [Originally Added On: March 17th, 2025]
- 0004) Supplements for Andropause: Enhancing American Men's Health and Vitality [Last Updated On: March 18th, 2025] [Originally Added On: March 18th, 2025]
- 0005) Navigating Andropause: Emotional Symptoms and Support Strategies for American Men [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0006) Managing Andropause: Diet, Exercise, Stress, Sleep, and Regular Check-ups for American Men [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0007) Andropause and Cognitive Health: Strategies for American Men to Maintain Mental Sharpness [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0008) Andropause: Understanding Male Menopause and Embracing Life Changes [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0009) Andropause in American Males: Understanding and Managing Diabetes Risk [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0010) Managing Andropause: Symptoms, Medical Advice, and Treatment Options for Aging Men [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0011) Andropause: Mental Health Strategies for Aging American Men [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0012) Andropause: Importance of Regular Check-ups for Men's Health and Well-being [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0013) Navigating Andropause: Emotional Strategies for American Men's Well-being [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0014) Andropause and Memory: Strategies for American Males to Enhance Cognitive Function [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0015) Andropause and Depression: Recognizing Signs and Seeking Help for American Men [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0016) Hydration's Crucial Role in Managing Andropause Symptoms in American Men [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0017) Andropause: Managing Symptoms to Balance Work and Health in American Men [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0018) Managing Andropause: Essential Foods for American Males' Health and Vitality [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0019) Andropause and Vision: Understanding Changes and Managing Eye Health in American Males [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0020) Andropause in American Men: Combating Fatigue with Exercise, Diet, and Medical Strategies [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0021) Andropause: Family Support Crucial for Men's Health and Well-being [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0022) Andropause and Hormone Replacement Therapy: Benefits and Risks for American Men [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0023) Andropause: Navigating Male Menopause with Support and Understanding [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0024) Andropause: Navigating Social Impacts and Maintaining Connections in American Men [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0025) Andropause and Blood Pressure: Monitoring and Management Tips for American Males [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0026) Andropause and Skin Health: Skincare Strategies for American Males [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0027) Andropause: Managing Mental Health with Strategic Mental Health Days [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0028) Andropause and Hair Loss: Causes, Diagnosis, and Treatment Options for American Males [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0029) Andropause: Declining Testosterone and Its Impact on Kidney Health in American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0030) Andropause and Digestive Health: Symptoms, Management, and Medical Advice for American Males [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0031) Managing Andropause: Exercise, Nutrition, and HRT for American Males' Muscle Health [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0032) Andropause and Liver Health: Strategies for American Males [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0033) Managing Andropause: Effective Stress Reduction Strategies for American Men [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0034) Andropause: Understanding Male Menopause and Managing Its Effects [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0035) Managing Andropause: Benefits of Exercise and Diet for Aging American Men [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0036) Andropause and Thyroid Function: Interconnected Health Issues in Aging American Men [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0037) Andropause and Cholesterol: Managing Lipid Levels in Aging American Males [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0038) Andropause and Joint Health: Strategies for American Men [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0039) Andropause in American Males: Impacts and Management of Respiratory Health [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0040) Andropause and Sleep: Managing Symptoms in American Men Through Holistic Approaches [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0041) Andropause and Emotional Intelligence: Navigating Male Menopause in American Men [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0042) Andropause: Impact on American Men's Self-Esteem and Treatment Options [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0043) Andropause: Understanding Male Menopause and Its Impact on Energy and Vitality [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0044) Andropause in American Men: Symptoms, Diagnosis, and Holistic Management Strategies [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0045) Andropause: Understanding Symptoms, Importance of Screenings, and Proactive Health Management for Men [Last Updated On: March 29th, 2025] [Originally Added On: March 29th, 2025]
- 0046) Mindfulness: A Holistic Approach to Managing Andropause in American Men [Last Updated On: March 29th, 2025] [Originally Added On: March 29th, 2025]
- 0047) Andropause: Understanding Male Menopause and Its Impact on Motivation and Well-being [Last Updated On: March 29th, 2025] [Originally Added On: March 29th, 2025]
- 0048) Andropause and Immune Health: Strategies for American Males [Last Updated On: March 29th, 2025] [Originally Added On: March 29th, 2025]
- 0049) Andropause: Understanding Symptoms, Treatments, and Maintaining Confidence in American Men [Last Updated On: March 29th, 2025] [Originally Added On: March 29th, 2025]
- 0050) Andropause and Hearing Loss: Understanding the Link and Managing Symptoms [Last Updated On: March 30th, 2025] [Originally Added On: March 30th, 2025]
- 0051) Andropause and Dental Health: Essential Tips for American Males [Last Updated On: March 30th, 2025] [Originally Added On: March 30th, 2025]
- 0052) Andropause: Enhancing Men's Quality of Life Through Community Support and Awareness [Last Updated On: March 30th, 2025] [Originally Added On: March 30th, 2025]
- 0053) Hobbies: A Vital Tool for Managing Andropause in American Men [Last Updated On: March 31st, 2025] [Originally Added On: March 31st, 2025]
- 0054) Managing Andropause and Allergies: A Comprehensive Guide for American Males [Last Updated On: April 1st, 2025] [Originally Added On: April 1st, 2025]
- 0055) Andropause: Impact on Creativity and Cognitive Function in Aging American Men [Last Updated On: April 2nd, 2025] [Originally Added On: April 2nd, 2025]
- 0056) Navigating Andropause: Goal Setting for Health and Resilience in American Men [Last Updated On: April 5th, 2025] [Originally Added On: April 5th, 2025]
- 0057) Andropause and Skin Sensitivity: Management Tips for American Men [Last Updated On: April 6th, 2025] [Originally Added On: April 6th, 2025]
- 0058) Andropause: Understanding Male Menopause and Its Impact on Purpose and Well-being [Last Updated On: April 7th, 2025] [Originally Added On: April 7th, 2025]
- 0059) Technology's Role in Managing Andropause: Wearables, Telemedicine, and AI Solutions [Last Updated On: April 7th, 2025] [Originally Added On: April 7th, 2025]
- 0060) Andropause Impact on Foot Health: Symptoms, Risks, and Management Strategies for Men [Last Updated On: April 8th, 2025] [Originally Added On: April 8th, 2025]
- 0061) Andropause and Time Management: Strategies for American Men to Thrive [Last Updated On: April 8th, 2025] [Originally Added On: April 8th, 2025]
- 0062) Andropause Effects on Nail Health: Strategies for American Males [Last Updated On: April 9th, 2025] [Originally Added On: April 9th, 2025]
- 0063) Andropause Effects on Hand Health: Strategies for American Males [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0064) Volunteering: A Holistic Approach to Managing Andropause in American Men [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0065) Andropause Impact on Eye Health: Dry Eye, Cataracts, AMD in American Males [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0066) Andropause: Impact on American Men's Adventure and Lifestyle Management Strategies [Last Updated On: April 11th, 2025] [Originally Added On: April 11th, 2025]
- 0067) Travel as Therapy: Managing Andropause Symptoms in American Men [Last Updated On: April 12th, 2025] [Originally Added On: April 12th, 2025]
- 0068) Andropause and Lifelong Learning: Enhancing Men's Health and Well-being [Last Updated On: April 12th, 2025] [Originally Added On: April 12th, 2025]
- 0069) Andropause and Ear Health: Strategies for American Males to Maintain Auditory Function [Last Updated On: April 15th, 2025] [Originally Added On: April 15th, 2025]
- 0070) Andropause Management: Harnessing Music Therapy for American Men's Holistic Health [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0071) Andropause and Nasal Health: Symptoms, Management, and Impact on American Males [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0072) Andropause Impact on American Men's Humor: Coping Strategies and Support [Last Updated On: April 17th, 2025] [Originally Added On: April 17th, 2025]
- 0073) Andropause: Understanding Male Menopause and Its Impact on American Men's Identity [Last Updated On: April 17th, 2025] [Originally Added On: April 17th, 2025]
- 0074) Art Therapy: A Holistic Approach to Managing Andropause in American Men [Last Updated On: April 18th, 2025] [Originally Added On: April 18th, 2025]
- 0075) Andropause: Navigating Male Menopause Through Social Connections and Open Dialogue [Last Updated On: April 18th, 2025] [Originally Added On: April 18th, 2025]
- 0076) Andropause and Throat Health: Symptoms, Management Tips, and Lifestyle Adjustments for American Men [Last Updated On: April 19th, 2025] [Originally Added On: April 19th, 2025]
- 0077) Andropause: Financial Planning and Lifestyle Adjustments for American Men's Health [Last Updated On: April 19th, 2025] [Originally Added On: April 19th, 2025]
- 0078) Andropause Effects on Tongue Health: Symptoms, Management, and Hormonal Therapy Insights [Last Updated On: April 19th, 2025] [Originally Added On: April 19th, 2025]
- 0079) Andropause Impact: Rising Depression and Anxiety Rates in American Males Over 20 Years [Last Updated On: April 22nd, 2025] [Originally Added On: April 22nd, 2025]
- 0080) Andropause: Understanding Male Menopause and Its Mental Health Impacts in American Men [Last Updated On: April 22nd, 2025] [Originally Added On: April 22nd, 2025]

List of USA state clinics - click a flag below for blood testing clinics.
Word Count: 398